CAR Cells, Revved Up
Jeffrey Laurence, M.D., and Rowena Johnston, Ph.D.
Research Question
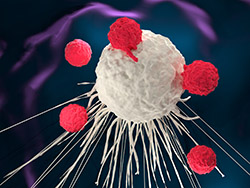
Photo © Meletios Verras I Dreamstime.com
Immunotherapies based on genetically engineered T cells, known as CAR T cells, are highly successful in curing certain types of cancer. Their potential efficacy as a component of an HIV cure is now a focus of intense interest. In a recent update, we discussed new evidence from amfAR grantee Scott Kitchen that HIV-specific CAR T cells prepared from gene-modified adult stem cells can form T cells capable of killing HIV-infected cells. They can also travel to, and persist in, common HIV reservoir sites.
Given this success, Dr. Kitchen sought to determine if those cells could be enhanced with improvements on three fronts: 1) an increased ability to differentiate into mature, HIV-fighting cells; 2) enhanced resistance to infection and destruction by HIV; and 3) with improved anti-HIV capabilities.
Findings
“Second generation” CAR cells were prepared and tested in humanized mice that are susceptible to HIV infection. The CAR cells were designed with a modification to the targeting gene (CD4) that would prevent their own infection by HIV. This modification allowed CAR cells to mature more normally than CAR cells with the unmodified version of CD4. The modified CAR targeted HIV infection as effectively as traditional CAR cells, and those animals that received the modified cells produced 10 times less virus than untreated mice following an HIV infection. They also had much faster clearance of the virus in combination with antiretroviral therapy, and much longer persistence as compared to earlier, more traditional forms of CAR T.
Impact
The authors concluded that “Our CD4-based HSC-derived CAR therapy could provide a long term, enhanced anti-HIV-1 immunity … [it] could also be combined [in a] ‘kick-and-kill’ strategy to reduce and eliminate HIV-1 reservoir.”
amfAR’s Role
amfAR was a funder of this research.
Original Article
http://www.ncbi.nlm.nih.gov/pubmed/33793675
Dr. Laurence is amfAR’s senior scientific consultant and Dr. Johnston is vice president and director of research.
Share This: