New Studies Advance HIV Cure Science
Researchers report new findings on post-treatment control, HIV reservoirs, and early treatment in children
At the 31st annual Conference on Retroviruses and Opportunistic Infections (CROI) in early March in Denver, Colorado, Adam Castillejo (aka the London Patient), the second person cured of HIV, opened the conference by championing the importance of collaboration between the HIV and the scientific communities and calling on researchers to prioritize progress toward a cure for HIV.
Some conference participants exemplified exactly what Castillejo talked about, with researchers, including amfAR grantees, sharing exciting developments in HIV cure science.
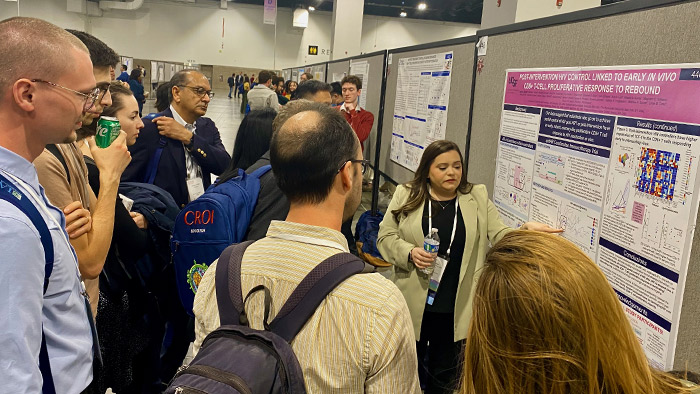
What Happens When HIV Rebounds
Last year at CROI, results from a complex amfAR-funded trial showed that individuals living with HIV may be able to control HIV when they stop ART as part of a combination immunotherapy. The trial combined five interventions: an HIV DNA vaccine, the immune hormone IL-12, a vaccinia boost vaccine, broadly HIV neutralizing antibodies, and a drug to activate the immune protein TLR9
While almost all participants showed signs that the virus persisted during the initial analytic treatment interruption, seven of the 10 did not rebound in the usual way, where a rapid burst of uncontrolled viral growth would be expected. Instead, they were able to control the virus in the absence of antiretroviral therapy (ART). Five of the seven participants had some level of HIV control for at least 100 days off ART, and one of the seven had no detectable virus for 18 months off ART.
Two new studies separately examined two of these factors: broadly neutralizing antibodies (bNAbs) and CD8+ T cells. Both studies were conducted at the lab of Dr. Rachel Rutishauser of the University of California, San Francisco (UCSF), an amfAR grantee and a principal investigator of the abovementioned cure trial.
One study examined how bNAbs functioned in the amfAR cure trial. In this analysis, Dr. Amelia Deitchman and colleagues found that, while higher bNAb exposure was associated with delayed viral rebound, bNAb exposure and the susceptibility of HIV to being neutralized could not be consistently linked to post-treatment control.
In light of these results, researchers suggest immunologic changes contribute significantly to post-treatment control. This was explored in another study that examined the role of CD8+ T cells, sometimes known as the foot soldiers of the immune system for their ability to expand in number to fight against viral and bacterial infections.

Previous studies have described a rapid increase of in HIV-specific CD8+ T cells in elite controllers (people living with HIV who control infection in the absence of ART), one feature that differentiates them from people living with HIV whose virus is not controlled without the help of ART. But, until now, this HIV-specific CD8+ T cell phenomenon had been noted only in the lab.
Along with other researchers, lead author Demi A. Sandel of UCSF analyzed this phenomenon in the amfAR-funded combination immunotherapy trial and a separate study and found that CD8+ T-cells proliferated early and robustly in participants. The results support continued focus on developing HIV cure strategies that enhance the capacity of HIV-specific CD8+ T cells to increase.
Early Treatment in Children
Years ago, the case of the Mississippi baby suggested that starting ART early in children who had acquired HIV in the womb might confer remission of the virus. Although that child experienced viral rebound after 27 months off treatment when not in care, a new study provides proof of concept that early treatment may reduce the HIV reservoir and lay the groundwork for a functional cure, particularly for children.
Researchers monitored 54 infants who acquired HIV in the womb and initiated ART within 48 hours after birth. Among six children (median age: 5.5 years) who met eligibility criteria and underwent a closely monitored treatment interruption, two experienced viral rebound quickly but four have been able to sustain remission of HIV for at least a year.
Characterizing the HIV Reservoir
In another cure-related presentation, researchers in a first-of-its-kind study characterized variations in antiretroviral distribution (primarily dolutegravir, in this case) across the body. ART is able to inhibit HIV replication and suppress the virus to undetectable levels, but cannot eradicate the viral reservoir in various parts of the body, in part due to the ability of the drugs to penetrate different tissue and organ sites. In particular, the researchers found lower concentrations of the antiretroviral in the central nervous system, which is typically hard to reach because of the blood-brain barrier.
Curing HIV is likely to require the inclusion of human immune responses, but little is known about how these responses might effectively engage and target HIV reservoir cells.
Results from a new study, funded in part by amfAR, help detail the interplay of immune responses and the HIV reservoir in relation to biological sex, adding to what we know about women living with HIV on ART, who are largely underrepresented in HIV cure trials.

While researchers have established that biological sex impacts immune responses, sex-specific differences in the HIV reservoir among long-term ART-treated individuals remain unclear. In this study, lead author Dr. Toong Seng Tan of the Ragon Institute of MGH, MIT and Harvard and Brigham and Women’s Hospital in Boston, along with others including amfAR grantees Drs. Xu Yu, Mathias Lichterfeld, Phyllis Tien, Michael J. Peluso, and Jeffrey M. Jacobson, sought to understand these potential differences by looking at significant features of the HIV reservoir.
Study participants included 34 males and 30 females, all cisgender on long-term ART and with similar demographic backgrounds.
There does seem to be a sex-based difference in how the immune responses in treatment-experienced people drive the evolution of the HIV reservoir, researchers noted in their analysis. The reservoir in women was shown to have features associated with deeper latency—cells that are less susceptible to reactivation and more easily “locked.” Thus, women may be better able to achieve a state of HIV control, a prime reason to include women in cure studies.
Share This: