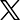Recent ARV Stockouts in India Created a Health Crisis for People Living with HIV
“ARV Is Our Lifeline. End Stockout Now,” read one sign taped to the wall of The National AIDS Control Organization (NACO) office in New Delhi, India. Protesters held a sit-in there between July 21 to August 31 to demand the government immediately restore the supply of antiretrovirals (ARVs) to people living with HIV (PLWH) nationwide. Letters and emails were sent to authorities for months, including national and international agencies, alerting them to the urgent situation and calling for action.

NACO claimed that 95% of PLWH were not facing any shortages during that period, but advocates disputed the accuracy of their data and emphasized that 5% still translated to 75,000 people being turned away from HIV treatment centers empty-handed.
In a communication sent to all State AIDS Control Societies as far back as May, NACO requested a change to existing regimens for PLWH as an interim measure to address the already growing nationwide stockout. Some were switched to different regimens as an interim measure, but without first checking an HIV viral load to check for pre-existing treatment failure or to guide future management.
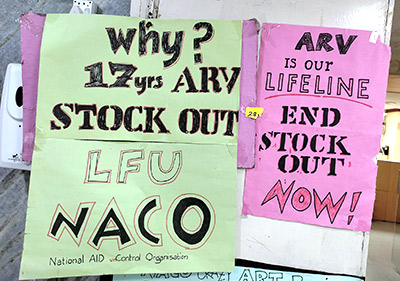
The stockout affected dosing as well. Instead of being given a one-month supply, they were given only enough ARVs to last a week or two, resulting in individuals coming back four or five times a month to obtain their medicines. For those taking abacavir, which was in even shorter supply, PLWH had to pay higher prices for their medicines at local pharmacies. A stockout of one particular form of the ARV dolutegravir meant that PLWH who needed it for second- and third-line therapies could not access it.
Some adults were offered pediatric formulations as a way to continue on the same ARVs, which increased the pill burden from one pill a day to 10 or more. In contrast, some children were given adult versions of lopinavir/ritonavir, because of a shortage of pediatric formulations for that ARV.
“Twenty years ago, there was no treatment in India. Now we have about [1.5 million] accessing treatment. That’s a big change,” says Loon Gangte, founder and president of Delhi Network of Positive People (DNP+), an amfAR community partner. According to UNAIDS, 2.4 million people are living with HIV in India. Of the 1.9 million who know their status, approximately 65% are on treatment. An estimated 1.3 million have achieved viral suppression. “Everyone has personal challenges [accessing healthcare] but this isn’t personal. The stockout shouldn’t have happened.”
“It’s been 17 years now since we’ve had treatment rollout in India [and this problem] has been recurring. I call it a chronic virus,” says Gangte. “People say HIV is the chronic virus, but the chronic virus is the stockout.”
Stockouts and shortages of ARVs and other HIV-related supplies have happened before, notably in 2014 and 2017. It’s seemingly not a problem with local production but more about missed timeframes in the initiation and completion of procurement processes.

Gangte was frustrated that NACO continually asked the protestors to disband prior to the shipment of ARV supplies starting on August 31. “That’s what I tell NACO: Okay, we will call off our protest but can you tell the virus in our body not to do any harm until next month, until you sort out this shortage?…No. The virus won’t simply listen. Every day we have to take our medicine on time. No matter what. Rain or shine. There’s no holiday. We’re not going to call off the protest unless our demands are met. Our demands are simple: Everyone gets medicine according to the NACO guidelines.”
Members of DNP+ endured 42 days in front of the NACO office, demanding appropriate supplies of ARVs for PLWH. Over that time, many PLWH made multiple visits to HIV treatment centers to collect their life-saving medicines while medical staff also had to cope with the increased number of visits. Time will tell how this stockout has impacted the risk of future treatment failures and the strength of the immune systems of those who struggled to maintain access to their medicines. Stock shortages or complete stock-outs must be avoided through consistent planning and effective implementation of national procurement processes.
Share This: